Iron Deficiency Anemia: Are Calcium Salts and Dairy Products One of the Causes?
It's very common to see people who combine calcium and iron food sources. Some physicians disagree with this habit. But why? Let's find out.

Abstract
It’s very common to see people who accompany foods rich in iron like meats and leafy greens with yogurt that is rich in calcium in the same meal, but some physicians are used to tell their patients with iron deficiency anemia to avoid such eating habit because they think depending on some experimental and epidemiological evidence that calcium inhibits iron absorption in intestines, and like so if the patient takes iron supplements and calcium supplements they also tell them to take supplements separately in different times. So are studies still with the same constant thought or changed? (article continues below)

Introduction
Iron is very abundant in foods, and it’s of two forms, heme and non-heme iron. Heme iron, the well absorbed form, comprises 40-45% of the iron in meat. Non-heme iron, the less-well to be absorbed, comprises the rest of iron in meat and the iron in plant sources like vegetables and grains.
It’s believed that there are inhibitors of iron absorption like phytates, polyphenols, and calcium. However, phytates and polyphenols inhibit only non-heme iron absorption, while calcium inhibits both heme and non-heme iron absorption.
Iron absorption in intestines
The physical state of iron affects its absorption process that occurs in the duodenum and proximal jejunum of small intestines. The absorbed iron is the iron in ferrous state (Fe2+) or that is bound to a heme. While for ferric iron (Fe3+), the form that mostly found in plant sources, to be absorbed, it must be reduced by duodenal cytochrome B (Dcytb) into ferrous iron. [1]
Heme iron uptake into enterocytes is mediated by intestinal heme transporter found on the enterocyte apical membrane in the duodenum, and non-heme iron is absorbed by Divalent metal transporter 1 (DMT1).
Iron efflux into plasma occurs through the transmembrane protein ferroportin (Fpn) that is expressed on the basolateral membrane of enterocytes in the duodenum.
Incorporation of iron with transferrin that mediates its transport through blood plasma requires it to be oxidized again into ferric (Fe3+) iron by ferroxidase which is hephaestin (Heph) that colocalize Fpn on the basolateral membrane (Fig1). [2]
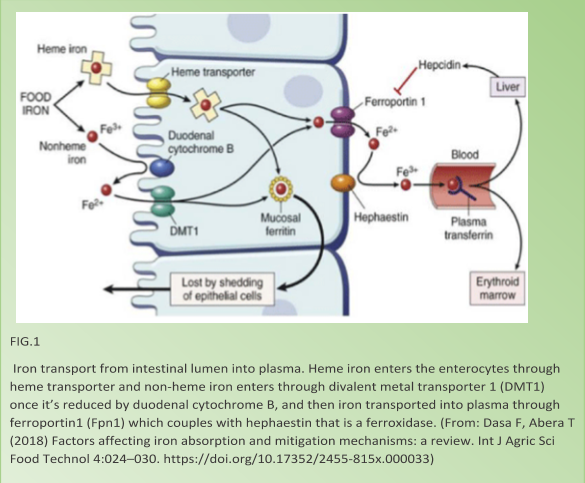
Calcium absorption in intestines
It occurs either through cells (transcellularly) or through the intercellular space between the cells (paracellularly). The transcellular transport occurs in the duodenum and it depends on calcitriol and the intestinal vitamin D receptor (VDR), while the paracellular transport occurs during higher calcium intakes along the whole small intestines; the duodenum, jejunum, and ileum. [3]
Effect of Calcium on iron absorption
Studies have succeeded to show an effect on direct measurements of iron absorption when it’s given with calcium but failed to show an effect when comparison is based on serum ferritin concentration changes. For example, in a study that is done on 21 females, they gave them non-heme iron that is labeled with radioisotopic iron in the 10-period days comparing two identical periods when calcium was distributed in two different ways, either in breakfast and late evening or in all meals. The research reported that 30-50% more iron is absorbed when no calcium sources were with meals. [4]
While in a randomized controlled study that is done on 109 healthy, free-living, premenopausal women in which 52 women assigned to be in the control group and 57 to receive two tablets of 250mg calcium with 2 meals daily for duration of 12 weeks, there was no significant difference on plasma ferritin concentration, or other iron status indicators. [5]
In terms of calcium and iron supplementation separation in times while patient taking them, there was a study conducted on Bolivian school children to show if there is a difference in reducing iron deficiency anemia in school children when giving calcium and iron combined versus iron supplementation alone. After 3 months of follow up, it was found that the iron deficiency anemia dropped significantly to 3% in both groups. So researchers came up with a conclusion that combined supplementation of iron and calcium is equally effective like in iron supplementation alone. [6]

Mechanism of action
The effect of calcium on iron absorption may be in the uptake step into enterocytes affecting DMT1 at the apical membrane, or in the transfer step into the plasma affecting Fpn & hephaestin at the basolateral membrane. Amazingly, a study explored these probabilities in human intestinal cells cultured in monolayers, assessing the transporters abundance over two various points of time. Firstly, after 1.5 hours, calcium had no effect on iron uptake or DMT1, but it decreased the abundance of Fpn on the basolateral membrane resulting in increased enterocytes storage and decreased efflux. In the second place, after 4 hours, both DMT1 and Fpn increases. Thus the study suggested an adaptation process occurs with time, which explains why long term studies with calcium supplements show no effect on iron status. [7]
For infants and toddlers, studies show an effect of prolonged breastfeeding and high consumption of cow’s milk on iron deficiency anemia. For breast milk, it’s because it contains an adequate amount of iron to 6 months of age and then other sources of irons are essential. For cow’s milk, the most probable mechanism is its decreased iron density. A second mechanism is allergy problems and small intestinal bleeding. A third mechanism is calcium inhibition to iron absorption. [8],[9]
Conclusion
The effect of calcium salts and dairy products on iron absorption is short term since many studies failed to show a reduction in iron status indicators like serum ferritin levels on long term interventions, suggesting an adaptation process that could be the upregulation of iron transport mediators on enterocytes.
Editors Pick:

References
[1] Ems T, St Lucia K, Huecker MR. Biochemistry, Iron Absorption. [Updated 2020 Apr 30]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan.
[2] MacKenzie EL, Iwasaki K, Tsuji Y. Intracellular iron transport and storage: from molecular mechanisms to health implications. Antioxid Redox Signal. 2008 Jun;10(6):997-1030. doi: 10.1089/ars.2007.1893. PMID: 18327971; PMCID: PMC2932529.
[3] Bronner F. Mechanisms of intestinal calcium absorption. J Cell Biochem. 2003 Feb 1;88(2):387-93. doi: 10.1002/jcb.10330. PMID: 12520541.
[4] Gleerup A, Rossander-Hulthen L, Gramatkowski E, Hallberg L. Iron absorption from the whole diet: comparison of the effect of two different distributions of daily calcium intake. Am J Clin Nutr 1995;61:97–104.
[5] Sokoll LJ, Dawson-Hughes B. Calcium supplementation and plasma ferritin concentrations in premenopausal women. Am J Clin Nutr. 1992 Dec;56(6):1045-8. doi: 10.1093/ajcn/56.6.1045. PMID: 1442655.
[6] Miranda M, Olivares M, Brito A, Pizarro F. Reducing iron deficiency anemia in Bolivian school children: calcium and iron combined versus iron supplementation alone. Nutrition. 2014 Jul-Aug;30(7-8):771-5. doi: 10.1016/j.nut.2013.12.008. Epub 2013 Dec 15. PMID: 24984991.
[7] Lönnerdal B. Calcium and iron absorption--mechanisms and public health relevance. Int J Vitam Nutr Res. 2010 Oct;80(4-5):293-9. doi: 10.1024/0300-9831/a000036. PMID: 21462112.
[8] Dalili H, Baghersalimi A, Dalili S, Pakdaman F, Hassanzadeh Rad A, Abbasi Kakroodi M, Rezvany SM, Koohmanaei Sh. Is there any relation between Duration of breastfeeding and anemia? Iran J Ped Hematol Oncol. 2015;5(4):218-26. Epub 2015 Dec 10. PMID: 26985355; PMCID: PMC4779157.
[9] Ziegler, EkhardE. (2011). Consumption of cow's milk as a cause of iron deficiency in infants and toddlers. Nutrition reviews. 69 Suppl 1. S37-42. 10.1111/j.1753-4887.2011.00431.x.


